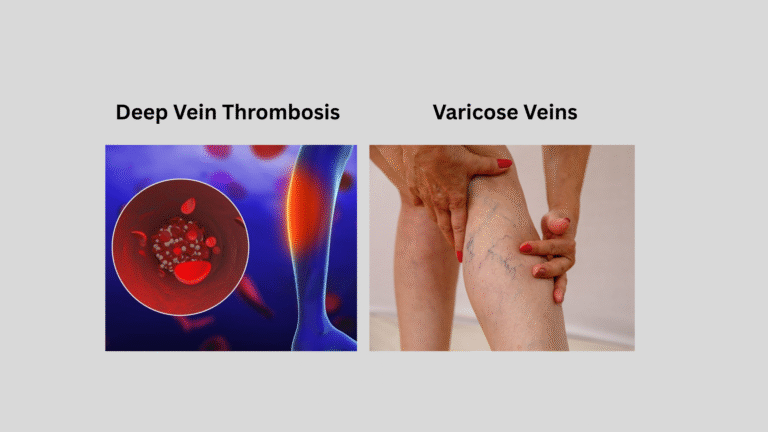
Understanding the Connection
Many people with varicose veins worry whether they might develop Deep Vein Thrombosis (DVT) — a serious condition where a blood clot forms in a deep vein, usually in the legs.
While both involve circulation problems, they are not the same disease. However, varicose veins can increase your risk of developing DVT under certain circumstances.
At Lumina Vein & Vascular Center, we help patients understand the difference — and guide them with preventive and treatment options tailored to their vascular health.
What Are Varicose Veins?
Varicose veins are swollen, twisted veins that develop when valves inside the veins fail to work properly. Blood pools in the veins, leading to visible bulges on the skin surface.
Common symptoms:
- Leg heaviness and pain
- Visible blue or green veins
- Swelling or itching around the veins
- Fatigue after standing for long periods
What Is Deep Vein Thrombosis (DVT)?
DVT occurs when a blood clot (thrombus) forms in the deep veins of the legs.
It’s a medical emergency because the clot can travel to the lungs, causing a pulmonary embolism (PE) — a potentially life-threatening condition.
Symptoms to watch for:
- Sudden leg swelling (usually one-sided)
- Warmth or redness in the leg
- Sharp pain or tenderness
- Difficulty walking
If you notice these symptoms, seek immediate medical care.
Are DVT and Varicose Veins Connected?
While not everyone with varicose veins develops DVT, the two can be linked.
Varicose veins cause slow or stagnant blood flow, which can increase the chance of clot formation.
Common risk factors shared by both conditions:
- Prolonged sitting or standing
- Obesity
- Pregnancy
- Hormonal therapy or birth control pills
- Family history of venous disease
- Lack of physical activity
Research suggests that people with chronic varicose veins have a higher risk (up to 5 times) of developing DVT compared to those without them.
Preventing DVT in Varicose Vein Patients
The good news? Prevention is possible.
Here’s how to keep your veins and circulation healthy:
✅ Stay active – Walking and leg exercises promote healthy blood flow.
✅ Wear compression stockings – These support your veins and reduce swelling.
✅ Avoid prolonged sitting or standing – Move every 30–60 minutes.
✅ Maintain healthy weight – Reduces strain on leg veins.
✅ Stay hydrated – Dehydration can make blood thicker and more prone to clotting.
Treatment Options at Lumina Vein & Vascular Center
Dr. Uday Ravi offers advanced, minimally invasive treatments that address the root cause of venous disease:
- Endovenous Laser Treatment (EVLT)
- Radiofrequency Ablation (RFA)
- VenaSeal Closure System
- Ultrasound-Guided Sclerotherapy
- Compression & Lifestyle Therapy
By correcting refluxing veins early, patients can reduce both symptoms and the risk of DVT complications.
Expert Insight: Dr. Uday Ravi
“Varicose veins don’t always lead to DVT, but they’re a signal that your venous system is under stress. Timely evaluation and treatment can prevent serious issues later.”
Dr. Uday Ravi MBBS MS FMAS FIAGES FISCP FALS FARIS DMAS (France)
Consultant Vascular & Laser Surgeon
When to See a Doctor
Seek immediate medical attention if you notice:
- Sudden increase in leg swelling or pain
- Skin redness, warmth, or hardness
- Shortness of breath or chest pain
Early diagnosis can save your life.
Takeaway
While DVT and varicose veins are different conditions, they share a common circulatory foundation. Managing varicose veins early helps protect your overall vascular health and lowers your risk of complications.
Trust Lumina Vein & Vascular Center — where modern laser treatments meet compassionate vascular care.
📞 Call: +91 88844 77725
🌐 Visit: luminaveincenter.com
👨⚕️ Lumina Vein & Vascular Center — Advanced Laser & Vascular Care